Asthma in Children
What Is Pediatric Asthma?
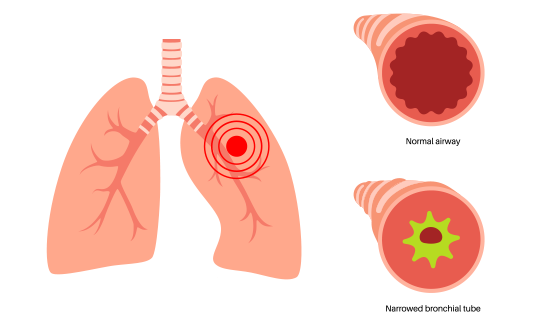
Asthma is a chronic condition that affects the airways in the lungs, making them inflamed and narrow. This causes difficulty breathing and can trigger wheezing, cough, chest tightness, and shortness of breath.
Asthma symptoms can come and go. With good care, your child can lead a healthy, active life.
Common Symptoms of Asthma in Children
Signs and symptoms of asthma in children can include:- Wheezing: A high-pitched sound when exhaling
- Coughing: Especially at night or early morning
- Shortness of breath: Difficulty breathing, even with simple activities
- Chest tightness: Sensation of pressure or heaviness in the chest
What Causes Asthma?
Researchers are not clear why some people get asthma and others do not, but it is likely due to some combination of environmental and inherited (genetic) factors.
People with asthma have inflamed airways which are sensitive to things that may not bother other people. These “triggers” cause the airways to constrict, or narrow.
Asthma Triggers
Triggers that may cause asthma episodes include:
- Allergens: Dust, pollen, mold
- Exercise: Physical activity, walking up and downstairs
- Respiratory infections: Colds, flu, and other common respiratory viruses
- Environmental irritants: Smoke, strong odors, cleaning products, construction, or pollution
Common Asthma Treatments
Two primary treatments for asthma include:
- Rescue inhaler (such as Albuterol or Xopenex). Fast-acting medicine for quick relief during asthma attacks. Use only as needed for coughing, wheezing, shortness of breath.
- Controller medicine. Taken daily to prevent symptoms and flare-ups (even if your child is not having any symptoms).
Why Use a Spacer with an Inhaler?

A spacer helps more medicine reach your child’s lungs. Children under 5 often use a spacer with a mask. Older children use a spacer with a mouthpiece.
- Easier to use (especially for young kids)
- More effective than inhaler alone
- Fewer side effects
When to Call the Doctor or Seek Help
Call 911 and go to the emergency room if your child:
-
Is having frequent asthma attacks and using their rescue inhaler more than every 4 hours
-
Has trouble talking, eating, or sleeping due to breathing
-
Is breathing very fast or hard
-
Is lethargic from coughing excessively
Call the doctor if your child:
-
Is visiting the school nurse once a week or more for breathing issues
-
Is having severe or uncontrolled symptoms, or if the child misses school due to frequent hospitalizations or urgent care visits due to asthma
-
Is not responding well to standard asthma treatment (it may take up to 3 to 4 weeks to see the effectiveness of a controller medication)
Pediatric Asthma Community Health Workers Program Facilitates Effective Asthma Management
RWJBarnabas Health’s Pediatric Asthma Community Health Workers Program aims to improve health outcomes of children with asthma by bridging gaps in care and promoting asthma trigger awareness and prevention. Our pediatric community health workers serve as a vital link between children and families and health care providers.
Our program focuses on connecting patients to pediatric pulmonologists and pediatric primary care physicians. Additionally, our community health workers emphasize education of home-based asthma triggers and access to essential services to reduce or eliminate asthma episodes. When a child visits one of our emergency rooms or is admitted to one of our hospitals, our doctors will connect a community health worker with the child and their family to help facilitate more effective asthma management.
Managing Asthma in School
Managing asthma in school can be challenging. Students should have access to their rescue inhalers and spacers for all inhalers regardless of age. Older kids may be qualified to carry and administer their own inhalers at school. An asthma action plan is provided by your doctor to inform both parents and school nurses on how to manage asthma including information on how to handle an asthma flare up and when to call 911.
Tips for Parents
- Follow the Asthma Action Plan you receive at your appointment.
- Avoid triggers like smoke, dust, pets or cold air.
- Use controller medicine as prescribed-even when your child feels well.
- Do not stop controller medications without your doctor's approval.
- Keep all follow-up appointments with your pulmonologist.
