It’s Possible To Feel Good And Stay Active, Even With A Diagnosis Of Heart Failure.
 The term “heart failure” means that this vital organ is damaged in some way. Despite the dire-sounding nature of the term, however, a diagnosis of heart failure is far from a death sentence.
The term “heart failure” means that this vital organ is damaged in some way. Despite the dire-sounding nature of the term, however, a diagnosis of heart failure is far from a death sentence.
“Care for heart failure patients has improved so dramatically that, although this is a chronic problem, patients who have it can live long and productive lives,” says Gary Rogal, MD, Chief of Cardiology for RWJBarnabas Health and a member of Barnabas Health Medical Group.
The key to this positive outcome is simple—but not necessarily easy. The heart failure patient must take medicine as directed and make the recommended lifestyle changes.
“The patient who listens to the things their doctor recommends they do will do better in the long term,” Dr. Rogal says. “I always tell my patients, ‘50 percent of your outcome is based on what I do, and 50 percent is based on what you do.’”
Understanding The Terms
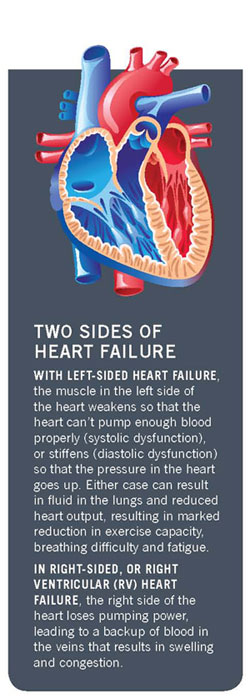
About 5.7 million U.S. adults ha ve heart failure, according to the Centers for Disease Control and Prevention. “ ‘Heart failure’ is a generic, umbrella term that covers many different disease entities,” Dr. Rogal says. “In the simplest terms, the heart is a pump, and it is failing as a pump.” The failure can fall into two different categories that often exist together: leftsided and rightsided dysfunction.
“People sometimes get confused when they hear ‘heart failure,’ and ask, ‘Am I going to have a heart attack?’” Dr. Rogal says. “The reality is that they ’re two different types of pathologies.”
Heart failure does not lead to a heart attack, he explains. Also, heart failure develops gradually, but a heart attack happens suddenly, when blood flow to an artery leading to the heart is blocked. In either case, patients will receive similar advice for a heart-healthy lifestyle.
Getting To Good Habits
Those recommendations likely come as no surprise: Take medication as directed. Exercise. Eat a healthy, low-salt diet. Stop smoking. Get enough sleep. Manage stress. Still, many patients don’t follow doctors’ orders, Dr. Rogal says. “People’s lives are so busy, and this tends to be a problem that’s not an immediate issue staring them in the face,” he says. “They think they can pay attention to it tomorrow.”
At the first sign of weakening or abnormality of the heart muscle, “I tell patients they need to start medications to help their heart muscle and begin to exercise,” Dr. Rogal says. “Walking is the easiest way to begin. And over the years, the pharmacology for heart failure has dramatically improved, so that we have a broad spectrum of medicines we can use.”
Dr. Rogal also recommends that patients with heart failure stop drinking. “Alcohol is a direct toxin to the heart muscle,” he says. “It can also lead to other issues, such as excessive sodium intake and dietary indiscretion. In my view, once you’ve started to develop any sign of heart muscle impairment, it’s time to hang up the alcohol.”
The same caution does not hold true for sexual activity. “In most cases, patients can remain sexually active,” Dr. Rogal says. “But be sure to discuss this with your doctor to ensure there are no limitations.”
Heart failure patients will find that the benefits of a heart-healthy lifestyle far outweigh the effort required to create new habits. Says Dr. Rogal, “You can live a very productive and positive life with heart failure—as long as you follow the guidelines shared by your doctor.”
Evaluating Heart Failure
Determining the degree of a patient’s heart failure allows doctors to make the best recommendations for preventing, delaying or treating the condition. Cardiologists put heart failure into one of four classes, starting with symptoms.
Here is the New York Heart Association Classification:
- CLASS I: Ordinary physical activity does not cause undue fatigue or shortness of breath
- CLASS II: Comfortable at rest, excessive physical activity results in fatigue and shortness of breath
- CLASS III: Symptoms with nonexcessive physical activity
- CLASS IV: Symptoms at rest The cardiologist will then do an objective assessment of the degree of heart failure based on observations as well as tests such as a blood test, X-ray, electrocardiogram, stress test and echocardiogram.