“I realized this is not going to kill you, this is not going to beat you. They always gave me that positive push.”

By his own admission, Norbert Perez is a stubborn man. He initially rebelled against the counseling he received after a diagnosis of Type 2 diabetes four years ago.
“They started giving me pills, but they weren’t working,” says Perez, 39, a forklift operator and Rahway resident. “They told me to change my eating habits, my lifestyle.
At first, I didn’t pay any attention to it. That typical man thing we do. We just go until we drop dead.”
But when a callus blistered and his foot swelled “beyond belief,” he ended up at the Center for Wound Healing and Hyperbaric Medicine at Robert Wood Johnson University Hospital (RWJUH) Rahway. The diagnosis: a diabetic foot ulcer.

“The first time we saw him, the wound was in very bad shape,” says podiatrist and wound care specialist Kyong Kim, DPM. “He had a bone infection, a nonhealing wound on the fifth metatarsal, from the bottom to the top of the foot, very extensive.”
“I was terrified because the first word that came out of everybody’s mouth was amputation,” Perez recalls. “I said, ‘No, I’m too young for that, you’re not amputating anything.’ I fought it.”
“We were all in to help this patient,” Dr. Kim says. “We decided to go with an aggressive treatment of debridement—the removal of dead tissue—and hyperbaric oxygen therapy.” A hyperbaric oxygen chamber puts a patient in a pressurized environment in which he breathes pure oxygen, which stimulates wound healing. The treatment was successful, and Perez was able to walk again.
A Near-Fatal Infection
However, Perez again failed to follow the lifestyle advice he was given. “Everything was working, but once again, I stopped following my orders,” he says. “I stopped checking my sugar level. I stopped taking my medicine. The infection came back. They had to treat it all over again. Took out a piece of the bone that was infected.”
The setback eventually led to a partial amputation of the foot, known as a transmetatarsal amputation.
“The infection was starting to get into my bloodstream, which could actually have been fatal,” Perez recalls. “That right there was what made me agree to the amputation. I pretty much lost half my foot.”
He credits the determination of the staff at RWJUH Rahway for the fact that he was able to get back on his feet in about a month, less than the predicted three-to-six-month recovery time. The wound care specialists worked closely with vascular surgeons to be sure blood flow would continue to circulate adequately. Perez was given a prosthetic filler with a carbon plate to replace the missing part of his foot, which allows him to walk in regular shoes.
“The team at Rahway continued to be there for me, even though I was the one messing up,” Perez says. “They still stood in there and helped me get through it. I think that’s what clicked that little button in my mind that made me realize, ‘You can do this.’” In addition to Dr. Kim, Perez says he formed an especially strong bond with podiatrist Sarah Haller, DPM.
“I realized this is not going to kill you, this is not going to beat you,” he says. “I don’t have to be on disability the rest of my life. They always gave me that positive push.”
Perez is back to work and preparing for a wedding with his fiancée, Charlene Marrow, who, he says, was also an essential part of his care team.
“I actually feel better now than before the amputation,” he says. “I’m still learning how to maintain—changing my eating habits, walking more.”
“Mr. Perez is not the only patient who has undergone this transformation,” says Dr. Kim. “When a person who had a wound like that for over a year is able to walk out, it makes us very happy. I study for them. I train for them. My grandmother has diabetes. It’s a great honor to do this.”
“The key to managing diabetes, I realized, is honestly, just love yourself and you’ll be fine,” Perez says. “It’s a matter of changing how you go about doing things. You just have to learn to moderate yourself. This last go-around was the final wake-up for me because I’m not even 40 yet. I’ve still got a lot of living to go.”
Foot Care for People With Diabetes
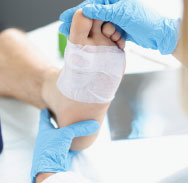 People with diabetes are more prone to wounds and wound infections in part because the disease compromises blood circulation in the skin and makes it more fragile. Feet are especially susceptible because the skin there encounters more weight and friction, according to Kyong Kim, DPM, a podiatrist at RWJUH Rahway’s Center for Wound Healing and Hyperbaric Medicine.
People with diabetes are more prone to wounds and wound infections in part because the disease compromises blood circulation in the skin and makes it more fragile. Feet are especially susceptible because the skin there encounters more weight and friction, according to Kyong Kim, DPM, a podiatrist at RWJUH Rahway’s Center for Wound Healing and Hyperbaric Medicine.
Warning signs for people with diabetes include ulcers or sores on the foot, leg or elsewhere; slow-healing wounds; black or brown tissue discoloration around a wound; pus or other fluid discharge; pain, redness or swelling.
The wound care team is ready for anything, Dr. Kim says. Treatment options include the latest in hyperbaric therapy, skin grafting, skin substitutes and more.
RWJUH Rahway offers a Diabetes Self-Management Program for people with diabetes or prediabetes. To learn more, call 732-499-6109. To learn more about the Center for Wound Healing and Hyperbaric Medicine, call 732-453-2915 or visit rwjbh.org/rahwaywoundcare.