"The bond we share ... no one can break it."

As a teen, Kimesha Smith couldn’t run as fast as her friends, but she didn’t think anything of it. Little did she know that she had a serious heart condition that would threaten her life.
When she was 18, Kimesha experienced shortness of breath. After a trip to a hospital near her home in Trenton, she was diagnosed with dilated cardiomyopathy, a weak heart. She was prescribed oral medications and did well initially.
In February 2020, she was transferred to Robert Wood Johnson University Hospital (RWJUH) in cardiogenic shock, a condition in which the heart is unable to pump enough blood to meet the body’s needs. Her liver and kidney function had deteriorated.
She was evaluated by a multidisciplinary team led by Deepa Iyer, MD, Heart Transplant Program Director at RWJUH and Assistant Professor of Medicine at Rutgers Robert Wood Johnson Medical School (RWJMS) specializing in Advanced Heart Failure, VAD and Transplant Cardiology; Hirohisa Ikegami, MD, Surgical Director of the Cardiac Transplant and VAD Program at RWJUH and Assistant Professor of Surgery, Division of Cardiac Surgery, at RWJMS; and Mark Russo, MD, MS, Chief of the Division of Cardiac Surgery and a member of RWJBarnabas Health Medical Group.

Kimesha’s physician team also included Anthony Lemaire, MD, Cardiac Surgery, and Kenneth Dulnuan, MD, and Danyaal Moin, MD, who specialize in Advanced Heart Failure, VAD and Transplant Cardiology.
Lifesaving Treatment
A temporary ventricular assist device (VAD) called Impella 5.5 was implanted in Kimesha by Dr. Ikegami and his team. At the time, RWJUH was one of only six hospitals in the country that had access to this device.
The VAD, which is implanted through an artery in the upper chest, pumps blood from the left ventricle of the heart into the aorta, the heart’s main artery, which carries blood to the rest of the body.
Kimesha was supported by the device for close to 70 days—one of the longest periods of time the device has ever been used. During that time, her liver and kidney function improved, and she was evaluated and placed on the heart transplant waiting list.
“She had a high level of antibodies in her blood, which limited her chances of getting a suitable donor heart,” says Dr. Iyer. “She had to undergo special treatments to remove and reduce those antibodies.”
Simultaneously, the COVID-19 pandemic had begun, so it was not only important to keep Kimesha stabilized until her transplant surgery but also to protect her from the virus. If she contracted COVID-19, the team would not be able to safely move forward with the transplant. Strict protocols were in place throughout the hospital, which included restricting visitors.
“Kimesha used FaceTime to communicate with her mother and aunt,” recalls Dr. Iyer. “This was the first time Kimesha was away from her mom, and she was very shy. The nurses in the Cardiovascular ICU went out of their way to make her feel comfortable. They braided her hair, played music, watched movies with her, decorated her room and drew pictures on the white board. These nurses became her family. Kimesha and her mom had such faith and optimism, which was inspiring to the entire care team. Her mom trusted the team to care for her daughter.”
Dr. Iyer remembers the day the team received the news that a donor heart was available.
“There must have been at least 20 caregivers standing outside her room to share the good news,” she says. “We all clapped and were cheering for her.” Kimesha was nervous. “I had been through so much,” she says.

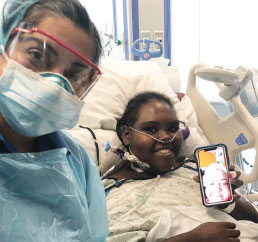
with Deepa Iyer, MD
A Remarkable Recovery
Procuring the donor heart was challenging due to the pandemic, says Dr. Ikegami.
“Surgeons from New Jersey and New York were not allowed to travel to certain statethe picture a nurse drew for Kimesha to decorate her rooms due to fears that they would bring COVID-19 with them,” he explains.
Fortunately, Dr. Lemaire was able to procure the organ, and on May 8, Dr. Ikegami performed the transplant. Kimesha was one of two patients to receive a heart transplant at RWJUH during the height of the pandemic, says Dr. Iyer. The other patient was discharged safely.
“Neither one of these transplants would have happened if we had inactivated our program during the pandemic,” says Dr. Iyer.

to decorate her room
Kimesha’s care required the coordinated efforts of a large multidisciplinary team, which included transplant cardiologists; transplant surgeons; certified nurse practitioners and registered nurses; cardiac anesthesiologists; cardiac perfusionists; critical care specialists; registered dietitians; pharmacists; social workers; cardiac rehabilitation therapists; hospital administrators and directors; and other medical professionals.
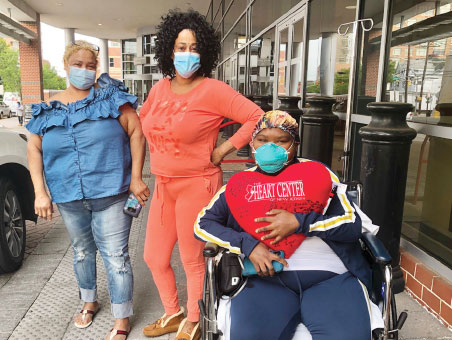
Kimesha was walking just five days after her transplant surgery. On May 18, just 10 days after the procedure, she went home.
Today, Kimesha has regular follow-up visits to ensure that her heart remains strong and healthy. Coordinated efforts continue to ensure that she receives the best care in a safe environment.
Kimesha is grateful. She sent Dr. Iyer and the transplant team a fruit basket with a note that said: “Thank you for being there for me. The bond we share ... no one can break it.”
Whoever your heart beats for, our hearts beat for you. At RWJBarnabas Health, we are the destination for ensuring your heart health. Learn more about the Advanced Heart Failure, VAD and Transplant Program at Robert Wood Johnson University Hospital, call (732) 253-3699 for more information or request an appointment.