Thoracic Outlet Decompression
Thoracic Outlet Syndrome (TOS) is a term used to describe a group of disorders that occur when there is compression, injury, or irritation of the nerves and/or blood vessels (arteries and veins) in the lower neck and upper chest area. Thoracic outlet syndrome is named for the space (the thoracic outlet) between your lower neck and upper chest where this grouping of nerves and blood vessels is found. Thoracic outlet syndrome affects people of all ages and gender. To relief the pressure exerted on the nerves and/or blood vessels, a thoracic outlet decompression may be performed.
Thoracic outlet decompression can be performed via the following methods: Non-Invasive (no incisions required / small puncture / low to moderate sedation), or minimally-invasive (small incisions of 2–3 inches long / general anesthesia). The type of method chosen will vary according to the specific type of TOS you have.
Types of Thoracic Outlet Decompression
Based on your specific-type of TOS, your doctor may recommend of the following options:
- Transaxillary Approach: Your doctor will make an incision in your chest to access the first rib, divide the muscles in front of the rib and remove a portion of the first rib to relive compression.
- Supraclavicular Approach: Your doctor will make an incision just under the neck to expose your brachial plexus region. Your doctor will then remove the muscles and a portion of the first rib causing the compression and potentially repair the compressed blood vessels.
- Intraclavicular Approach: Your doctor will make an incision under your collarbone and across your chest. This procedure may be used to treat compressed veins that require extensive repair.
- Robotic Approach: Your doctor will make a few small incisions in your chest. A robotic camera and small robotic instruments will be introduced. The procedure will remove a portion of the first rib and decompress the nerves and vessels of the thoracic outlet.
- Nerve Block Treatment: Nerve Block is a non-surgical alternative. It involves using botulinum toxin type A injections to provide temporary pain relief for patients.
How to Prepare for Thoracic Outlet Decompression Procedure
Before the procedure, your doctor and treatment team will explain to you what to expect before, during and after the procedure, and potential risks of the procedure. Talk to your doctor about:
- All medications, herbal products and dietary supplements you are currently taking and ask for their recommendations about each.
- Diabetes and how to adjust your medicine on the day of the procedure.
- Radiation exposure, especially for those that are pregnant.
- Any allergies to medicines, latex, tape, iodine, and anesthetic agents.
- Any history of bleeding disorders.
- Any implanted device (e.g. pacemaker or ICD).
- Any body piercings on your chest or abdomen.
Other recommendations include:
- Eat a normal meal the evening before the procedure. However, do not eat, drink or chew anything after midnight before your procedure. If you must take medications, only take them with sips of water.
- Leave all jewelry at home.
- Remove all makeup and nail polish.
- Wear comfortable clothing when you come to the hospital.
- If you normally wear dentures, glasses, or hearing devices at home, plan to wear them during the procedure.
What to Expect Before Thoracic Outlet Decompression Procedure
To determine whether you need either procedure, your doctor might perform a variety of diagnostic tests, including:
What to Expect During Thoracic Outlet Decompression Procedure
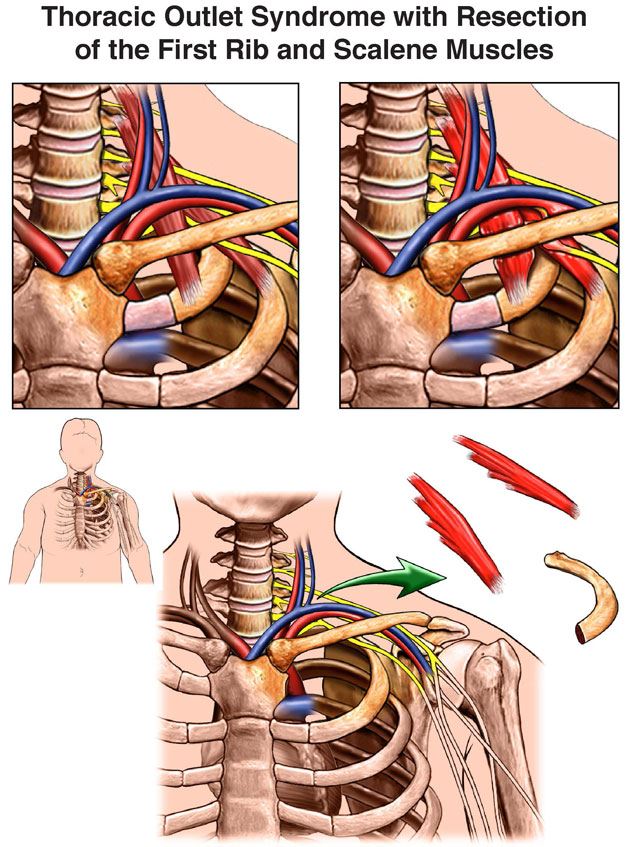
Medical Animation Copyright © 2019 Nucleus Medical Media, All rights reserved.
A thoracic outlet decompression surgery typically takes 2 hours to complete but the preparation and recovery time may add several hours. The procedure is usually done in cardiothoracic operating room (OR). Check with your doctor about the details of your procedure. In general, during TOS via a transaxillary approach:
- You will change into a hospital gown.
- A nurse will start the intravenous (IV) line in your arm which will administer medications, fluids, and also give you a sedative that will help you relax.
- Usually, your doctor will administer general anesthesia (make you feel sleepy).
- Once you are sedated, your doctor may insert a breathing tube through your throat into your lungs and connect you to a ventilator. This will breathe for you during surgery.
- Your doctor will make an incision above the clavicle or under the arm.
- Afterwards, your doctor will remove the extra rib and close the incision with stitches.
What to Expect After Thoracic Outlet Decompression Procedure
After this procedure, you will remain in the hospital for 1 to 3 days. Other recommendations include:
General Guidelines
- Your vital signs, such as your heart rate, breathing, blood pressure, and oxygen levels, will be closely monitored.
- You will probably have a tube draining the fluid from your heart or chest.
- You may feel some soreness, but you shouldn’t feel severe pain. Pain medications are available if needed.
- You will probably be able to drink the day after surgery. You can have regular foods as soon as you can tolerate them.
- Ambulation is started on the first or second day of surgery.
- You can probably do your normal activities after the surgery. But, you may need to take it easy at first. No heavy lifting or vigorous exercises until your body has healed.
- Your doctor will give you instructions to follow during your recovery.
